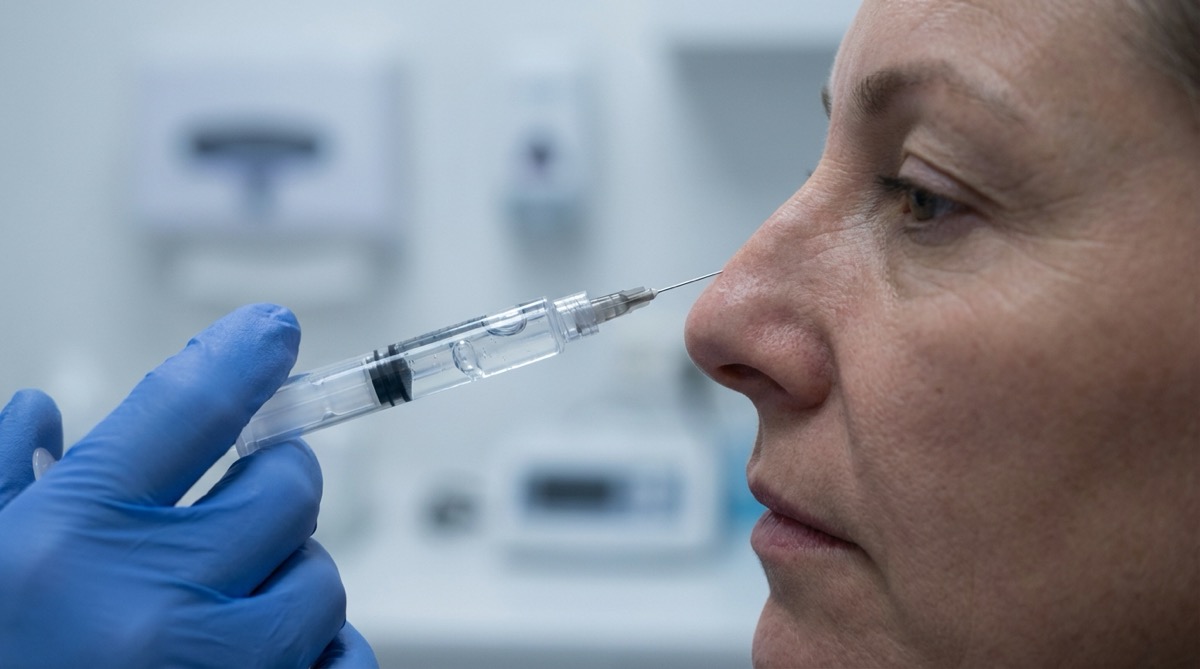
The idea of reshaping your nose without surgery sounds almost too good to be true — and in many ways, it is. Non-surgical rhinoplasty, often marketed as a “liquid nose job” or “5-minute nose job,” uses injectable hyaluronic acid fillers to alter the nose’s appearance. It is fast, requires no anesthesia, and has virtually no downtime. I understand the appeal.
But as a rhinoplasty specialist with over 20 years of experience and more than 8,000 nasal surgeries, I have also seen the consequences of this procedure gone wrong — and I have operated on patients whose non-surgical rhinoplasty created problems that were far more complex than the original concern they wanted to address. In this article, I want to give you an honest, evidence-based perspective on what non-surgical rhinoplasty can realistically achieve, what it absolutely cannot do, and the serious risks that are often minimized in marketing materials.
What Non-Surgical Rhinoplasty Can Do
Non-surgical rhinoplasty does have legitimate applications. When performed by an experienced injector who understands nasal anatomy deeply, fillers can achieve modest improvements in specific situations:
- Camouflage a dorsal bump: By injecting filler above and below a bony hump, the injector creates a smoother profile line. The bump is not removed — it is disguised by filling the areas around it.
- Improve minor asymmetries: Small depressions or irregularities on the nasal bridge can be smoothed with precise filler placement.
- Subtle tip refinement: A small amount of filler at the nasal tip can create a slight lifting effect or improve tip definition in carefully selected patients.
- Correct post-surgical irregularities: In some rhinoplasty patients, minor contour irregularities after surgery can be camouflaged with a touch of filler rather than a revision procedure.
These are real, valid uses. The key word in every case is “subtle.” Non-surgical rhinoplasty works by adding volume, and the nose is a small structure where even 0.1 ml of filler makes a visible difference.
What Non-Surgical Rhinoplasty Cannot Do
Here is where honest communication becomes critical, because the limitations are substantial:
It cannot make your nose smaller. This is the single most important limitation, and the one most frequently misunderstood. Fillers add volume. They can create optical illusions that make certain features less prominent, but the overall size of the nose either stays the same or increases. If your primary concern is that your nose is too large, non-surgical rhinoplasty is not the answer — it will make it bigger.
It cannot fix breathing problems. Nasal obstruction caused by a deviated septum, turbinate hypertrophy, or internal valve collapse requires surgical correction. Fillers placed externally have no effect on the internal airway. In fact, poorly placed fillers can worsen breathing by compressing the nasal passages from outside.
It is not permanent. Hyaluronic acid fillers are absorbed by the body over 6 to 18 months. This means the patient commits to repeat injections indefinitely to maintain the result. Over years, the cumulative cost can exceed the one-time cost of surgical rhinoplasty — with none of the permanence.
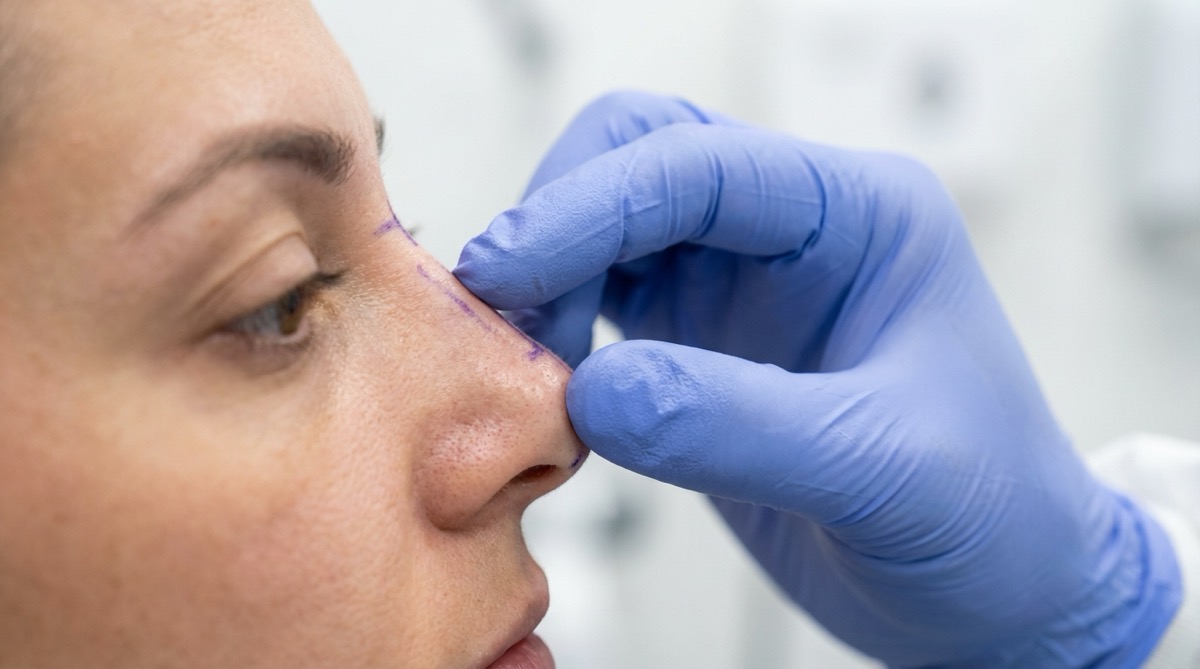
It cannot reshape bone or cartilage. The fundamental architecture of the nose — the nasal bones, the upper lateral cartilages, the lower lateral cartilages, the septum — remains completely unchanged. Fillers sit on top of these structures as a soft-tissue layer. They cannot narrow wide nasal bones, rotate a drooping tip, or correct a twisted nose.
It cannot address complex deformities. Saddle nose deformity, significant post-traumatic deviation, cleft lip nasal deformity, and other structural problems require cartilage grafting and precise surgical reconstruction — not filler injections.
The Serious Risks Nobody Talks About
The nose is one of the highest-risk areas for filler injection in the entire face. This is not opinion — it is vascular anatomy. The nose has a complex, highly variable blood supply with multiple anastomoses (connections between arteries). When filler is inadvertently injected into or around these vessels, the consequences can be devastating:
Vascular compromise and skin necrosis: If filler compresses or enters the blood vessels supplying the nasal skin, the tissue loses its blood supply. The skin turns white, then blue, then black as it dies. This can result in permanent scarring and tissue loss on the most visible part of the face. Treatment with hyaluronidase (the filler-dissolving enzyme) must begin within minutes to hours — and even then, outcomes are unpredictable.
Blindness: The nasal arteries communicate with the ophthalmic artery system that supplies the retina. Filler injected into the dorsal nasal artery can travel retrograde into the retinal vasculature, causing permanent, irreversible blindness. This is not a theoretical risk — it has been documented in peer-reviewed medical literature multiple times. The nose and glabella (area between the eyebrows) are the two highest-risk zones for filler-related blindness.
Stroke: In rare but documented cases, filler material reaching the cerebral vasculature has caused stroke. The interconnected arterial system of the face makes this anatomically possible whenever fillers are injected in the central face.
“The nose is a danger zone for fillers. Its blood supply is complex, variable between patients, and directly connected to the arteries that supply the eyes and brain. No amount of marketing can change vascular anatomy.”
When Fillers Become a Problem: The Filler Nose Syndrome
There is another risk that develops slowly over time, one that I see increasingly in my practice: filler nose syndrome. This occurs in patients who receive repeated filler injections over months or years. The cumulative effect creates a characteristic appearance:
- Progressive widening: The nose gradually becomes broader and more amorphous as filler spreads through the soft tissues. What started as a “quick fix” for a bump has made the nose wider and less defined.
- Loss of definition: The natural contours of the nasal tip and bridge become obscured under layers of accumulated filler. The nose takes on a smooth, puffy, unnatural appearance.
- Skin changes: Chronic filler presence can thin the nasal skin over time, making it more translucent and prone to showing irregularities. In some cases, the skin develops a bluish discoloration (Tyndall effect) from superficially placed hyaluronic acid.
- Fibrosis and granulomas: The body’s inflammatory response to repeated filler injections can create scar tissue (fibrosis) and granulomas — firm nodules that are difficult to treat and can distort the nose permanently.
The tragedy of filler nose syndrome is that it creates a problem that is harder to correct surgically than the original complaint. Rhinoplasty on a nose with extensive filler history involves working through scar tissue, fibrotic capsules, and unpredictable tissue planes. The surgical complexity — and risk — increases significantly.
When Surgical Rhinoplasty Is the Better Choice
For the vast majority of patients who are unhappy with the shape or function of their nose, structural rhinoplasty remains the gold standard. Here is why:
- Permanent results: A single surgery produces results that last a lifetime. No repeat treatments, no ongoing costs, no gradual loss of correction.
- True size reduction: Surgical rhinoplasty can actually make the nose smaller — narrowing the bridge, refining the tip, reducing alar flare — something fillers fundamentally cannot do.
- Functional improvement: Surgery can simultaneously correct breathing problems by addressing the septum, turbinates, and internal valves.
- Structural integrity: Cartilage grafts create a strong, lasting framework that supports the nose through decades of aging, rather than a temporary filler layer that will be absorbed.
- Natural aging: A well-structured nose ages gracefully with the face. A filler-dependent nose requires constant maintenance, and the appearance changes unpredictably as filler migrates and degrades.
Surgical rhinoplasty requires downtime — typically 7 to 10 days of social recovery and 3 to 6 months for swelling to fully resolve. But this investment of time yields a permanent transformation, whereas non-surgical rhinoplasty offers a temporary illusion that must be repeated indefinitely.
Frequently Asked Questions
Can non-surgical rhinoplasty make my nose smaller?
No. This is the most common misconception. Fillers add volume to the nose — they cannot remove tissue, narrow bone, or reduce cartilage. Strategic placement can create the illusion of a smoother profile by camouflaging a bump, but the nose becomes slightly larger overall. If reducing nose size is your goal, surgical rhinoplasty is the only effective option.
How dangerous are nose fillers really?
The nose is classified as a high-risk zone for filler injections due to its complex vascular anatomy. Documented complications include skin necrosis (tissue death), permanent blindness, and stroke. While these severe complications are rare, they are not theoretical — they occur in real clinical practice. The risk is higher with inexperienced injectors, but even experts have reported vascular events because of the unpredictable anatomical variations in nasal blood supply.
I had filler in my nose and want surgery now. Is that possible?
Yes, but there are important considerations. I recommend dissolving all filler with hyaluronidase and waiting at least 3 to 6 months before surgical rhinoplasty. This allows the tissues to return to their natural state and gives me the most accurate assessment of your nasal anatomy. Surgery on a nose with residual filler is more complex due to altered tissue planes and potential fibrosis.
Is non-surgical rhinoplasty a good “test run” before committing to surgery?
This is a common marketing claim, but it is misleading. Non-surgical rhinoplasty and surgical rhinoplasty achieve fundamentally different things. Filler adds volume and camouflages; surgery reshapes, reduces, and restructures. What you see after filler is not a preview of what surgery would achieve. A proper surgical consultation with computer imaging provides a far more accurate preview of potential surgical outcomes.
How much does non-surgical rhinoplasty cost over time compared to surgery?
A single non-surgical rhinoplasty session typically costs $600 to $1,500. Since results last 6 to 18 months, patients need 1 to 2 treatments per year indefinitely. Over 10 years, the cumulative cost ranges from $6,000 to $30,000 — often exceeding the one-time cost of a permanent surgical rhinoplasty. Add the ongoing time commitment, the cumulative risks of repeated injections, and the possibility of developing filler nose syndrome, and the cost-benefit analysis strongly favors surgery for most patients.
Making the Right Decision for Your Nose
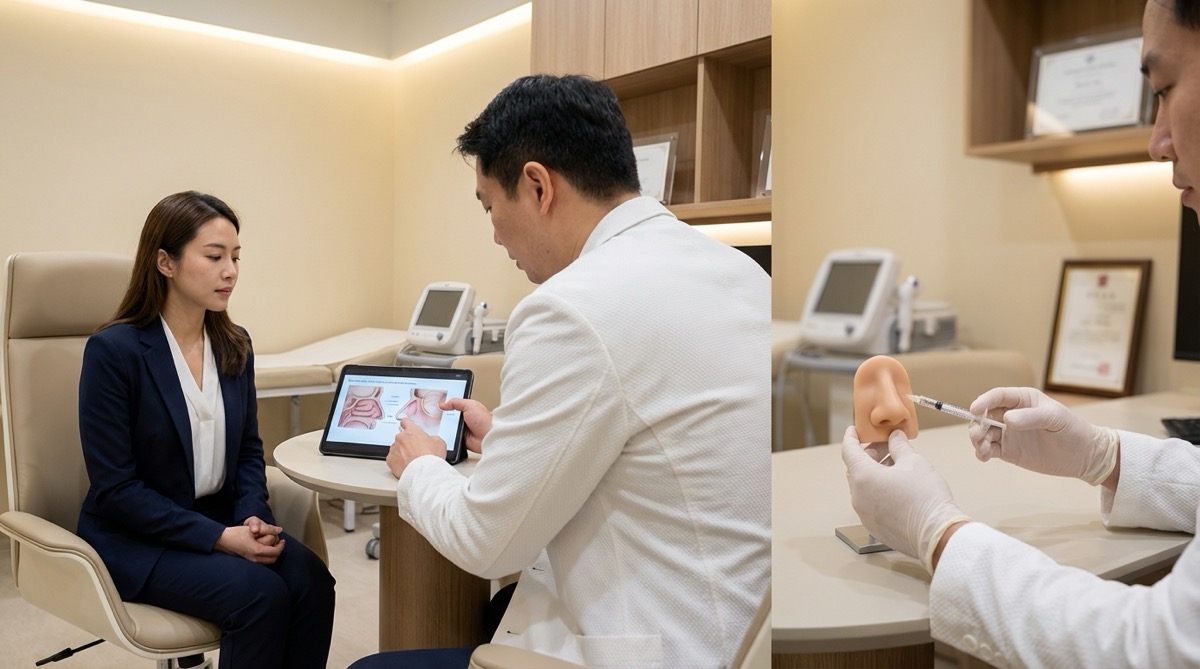
I am not against non-surgical rhinoplasty categorically. In the right patient, with the right expectations, performed by the right hands, it can be a reasonable option for minor, temporary corrections. But I believe every patient deserves complete, honest information before making this decision — including the limitations and risks that are too often glossed over.
If you are considering any form of rhinoplasty — surgical or non-surgical — I encourage you to schedule a consultation so we can evaluate your anatomy, discuss your goals, and determine which approach will truly serve you best in the long term.
Learn more about structural rhinoplasty or explore other facial procedures like the regenerative deep plane facelift.
Dr. Walter Zamarian Jr.
CRM-PR 17.388 | RQE 15.688
Board-Certified Plastic Surgeon — Londrina, PR, Brazil